Osteochondroses
AetiologyOsteochondroses are a group of 'diseases' of children and adolescents (typically) in which localized tissue death (necrosis) occurs, usually followed by full regeneration of healthy bone tissue. The singular term is osteochondrosis. (1) Osteochondroses are disorders of primary and secondary growth centres, or lesions at the apophyseal or epiphyseal growth areas of bones. (2)
During the years of rapid bone growth, blood supply to the growing ends of bones (epiphyses) may become insufficient, resulting in necrotic bone, usually near joints. Since bone is normally undergoing a continuous rebuilding process, the necrotic areas are most often self-repaired over a period of weeks or months.
Osteochondroses can affect different areas of the body and are often categorized by one of three locations: articular, non-articular, and physeal. (3)
Osteochondritis dissecans is a form of osteochondrosis in which loose bone fragments may form in a joint.
The EponymsMany theories have been advanced to account for osteochondrosis, but none has proven fully satisfactory. Stress and ischemia (reduced blood supply) are two of the most commonly cited factors. Athletic young children are often affected when they overstress their developing limbs with a particular repetitive motion. Many cases are idiopathic.
Freiberg's InfractionMost of the sites of osteochondrosis are known by eponyms. Amongst the Osteochondroses are the following.
Name Site Notes Kienböck's Disease lunate Legg-Calvé-Perthes disease hip- femoral head commonly known as Perthes Disease Scheuermann's disease spine (thoracic) Köhler's disease tarsal navicular Freiberg's Disease Second metatarsal head Commonly referred to as Freiberg's infraction because it was thought to relate to trauma Osgood-Schlatter Disease tibial tubercle - 10 and 15 yr and is usually unilateral - related to sports activity Panner's disease capitellum of the elbow Osteochondritis dissecans of the femoral condyle femoral condyle- usually medial condyle Sever's disease calcaneum Sinding-Larsen-Johansson syndrome inferior tip of patella
syn: Freidberg's Infarction, Freidberg's Disease
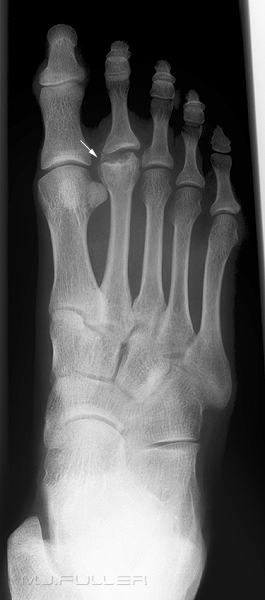
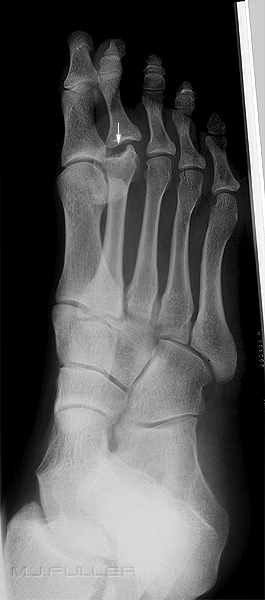
Osteochondritis Dissecans of the Femoral Condyle (OCD)This condition was first described by Freiburg in 1914 as an infarction of the second metatarsal head. Freidburg's has the potential to affect any of the metatarsal heads. Radiographically a characteristic flattening of the head of the metatarsal can be viewed. This characteristic feature is known as the 'egg crush' appearance. Furthermore, the metatarsal head is prone to flaring and a trumpet like appearance.
5 Stage Classification
- Stage 1 Epiphyseal fissure fracture
- Stage 2 Central portion of bone re-absorption
- Stage 3 Metatarsal head begins to flatten
- Stage 4 Intra- articular loose body
- Stage 5 Complete flattening of the metatarsal head (4)
Typical osteonecrosis of the head of the second metatarsal seen in Freiberg's infraction Note that central bone has undergone re-absorption.
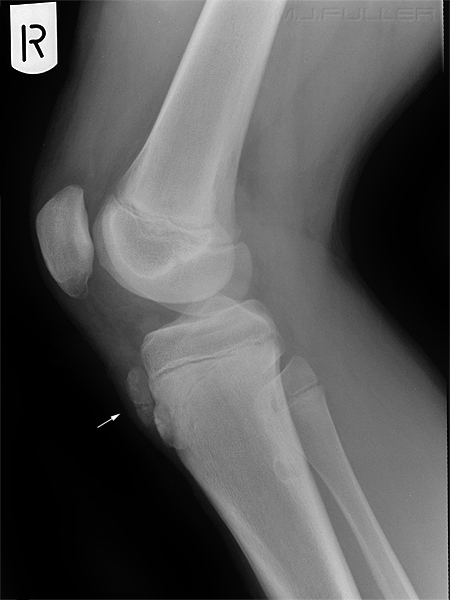
- OCD is a defect in the subchondral bone of a joint with partial or complete separation of the bone fragment;
- most often seen in the medial femoral condyle (about 80% of cases), and less often seen in posterior aspect of lateral condyle;
- is usually unilateral (74%)
- relatively common source of loose bodies in the knee or even an incongruous joint if the separated fragment is large;
- twice as common in males;
- classically occurs below the age of 18 (range: 6 to 53 years) (5)
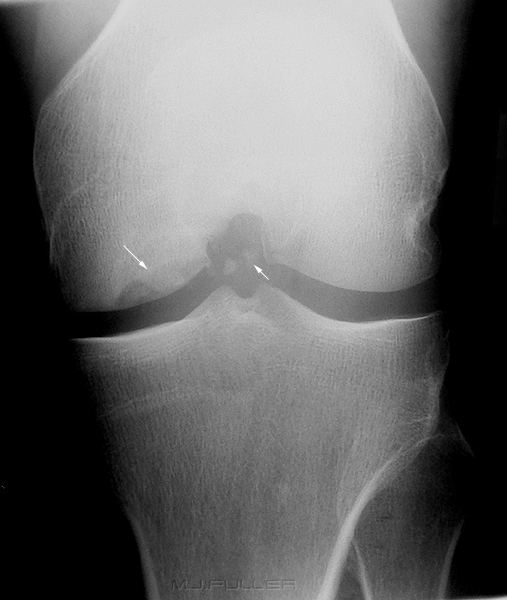
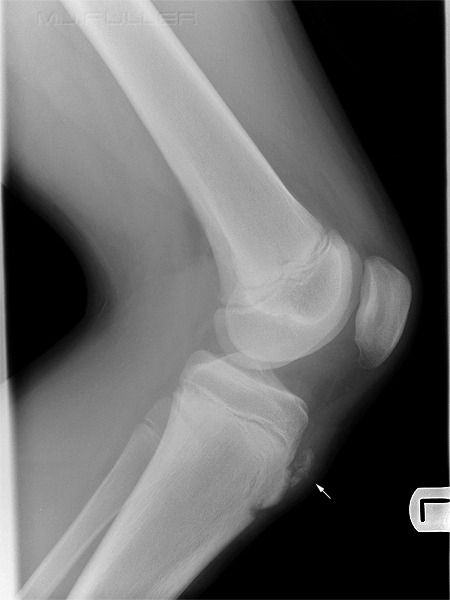
OCD of the medial femoral condyle. Note the subchondral bone defect (arrowed) in the medial femoral condyle and the associated loose bodies (arrowed)
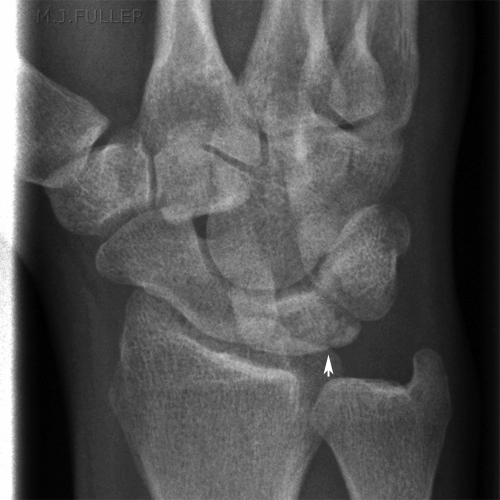
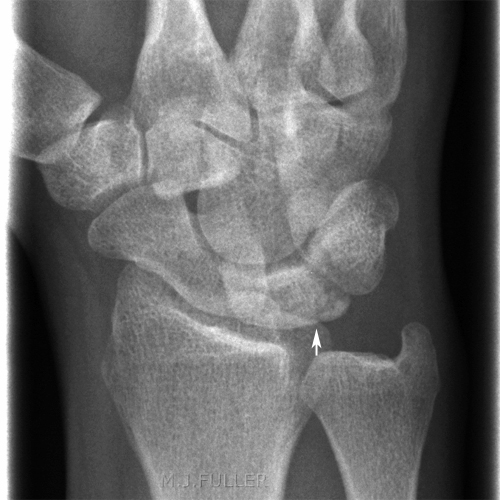
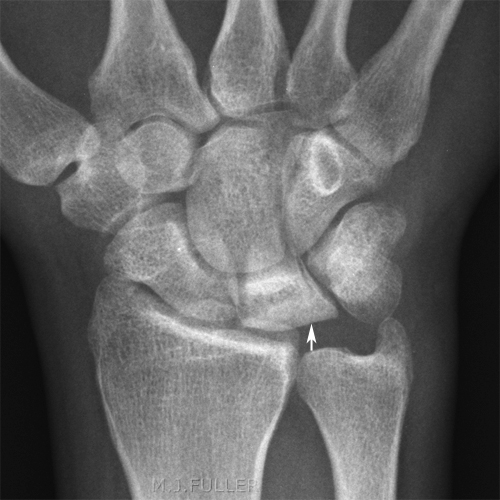
Kienbock's Disease
Kohler's Disease of the Tarsal Navicular- disease which involves collapse of the lunate due to vascular insufficiency and avascular necrosis;
- first described in 1910 by Kienbock (republished article in CORR 1980, Vol 149);
- disease occurs most often in young adults between 15 and 40 years;
- is usually unilateral;<a class="external" href="http://www.wheelessonline.com/ortho/kienbocks_disease_lunatomalacia" rel="nofollow" target="_blank">Wheeless' Textbook of Orthopaedics</a>Case 1
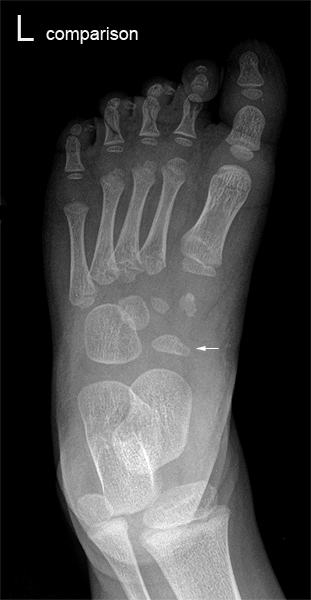
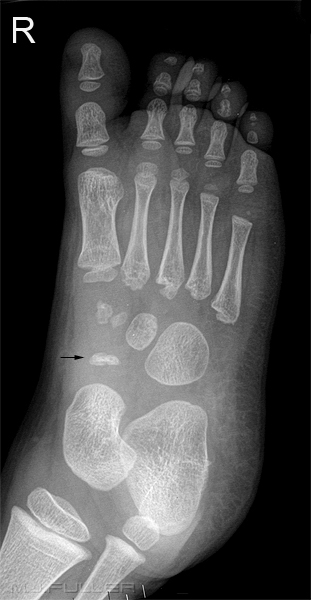
Osteochondrosis of the tarsal navicular was described by Köhler in 1908. It is defined as a clinical condition consisting of:
1) pain in the region of the tarsal navicular, and
2) radiographic changes consisting of increased radiodensity, fragmentation and eventual narrowing of the tarsal navicular. .
Clinical features:
- child younger than 6 presenting with midtarsal pain
- Boys & girls, 4:1 in most reported series
- Pain with weight bearing / relieved by rest
- palpable tenderness over navicular (6)
Osgood-Schlatters Disease
- type of juvenile traction osteochondritis;
- refers to partial avulsion of the tibial tuberosity (anterior surface of apophysis) which has no
involvement of tibial physis;
- usually occurs in late childhood or early adolescence;
- more common in boys;
- may represent an over use disease;
- condition occurs at a time when increasing demands are made on a still immature skeleton;
- repetitive stress on tuberosity may cause partial avulsion;
- a painful non union will develop, if intervening gap fills with fibrous tissue rather than bone; (7)
Legg-Calvé-Perthes disease (LCPD)
Note the prominence, irregularity and fragmentation of the tibial tuberosity (arrowed). Same patient- condition is bilateral.
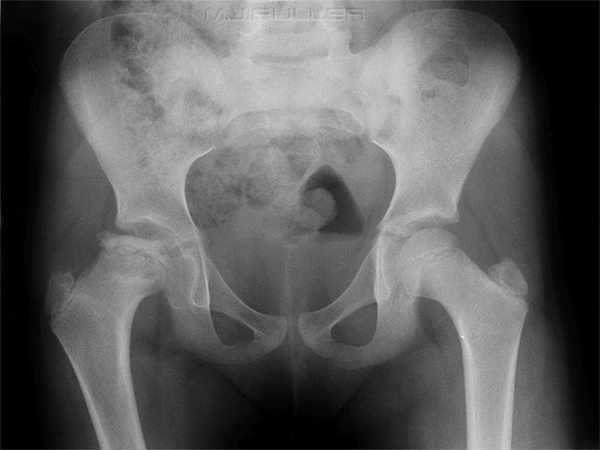
Legg-Calvé-Perthes disease (LCPD) is the name given to idiopathic osteonecrosis of the capital femoral epiphysis of the femoral head.
RadiographyIt is useful to produce comparable serial films. If you are not sure what views to do, check old imaging
- Initial investigation
AP Pelvis
- True AP
- Symmetrical internal rotation of femora
- gonad protection
Frogleg lateral
- a symmetrical positioning will facilitate comparison
- gonad protection
- Follow up
AP Pelvis or AP Hip
- True AP
- Symmetrical internal rotation of femora
- gonad protection
Lateral hip
- gonad protection
One of the earliest plain film features of Perthes disease is a subchondral fracture of the anterolateral aspect of the femoral capital epiphysis. This finding is best demonstrated on the frog-leg lateral projection.
Prognosis for the disease relates to the "ABC of Perthes"
A. Age of Onset <5 Years: almost all do well.
> 9 years: only 10-15% do wellB. Bone Growth <a class="external" href="http://www.bgf.asn.au/textbook/structure_fuction/macro_bone/physis/physis.html" rel="nofollow" target="_blank">Physeal</a> involvement increases the chance of a poor sphericity at maturity. C. Classification of extent of disease: >50% of head involved have a poor prognosis. (8)
Classification SystemsA number of classification systems have been used in Perthes disease, and these have largely been based on plain film appearances
- Catterall
- Herring
- Salter-Thompson
- Stulberg
Mortality/Morbidity
- LCPD is a self-limited disease if not treated.
- Outcome is extremely variable.
Prevalence/Incidence/Sex Distribution
Sex
- Males are affected 4-5 times more often than females.
Age
- LCPD most commonly is seen in persons aged 3-12 years, with a median age of 7 years.
Plain Film Appearances
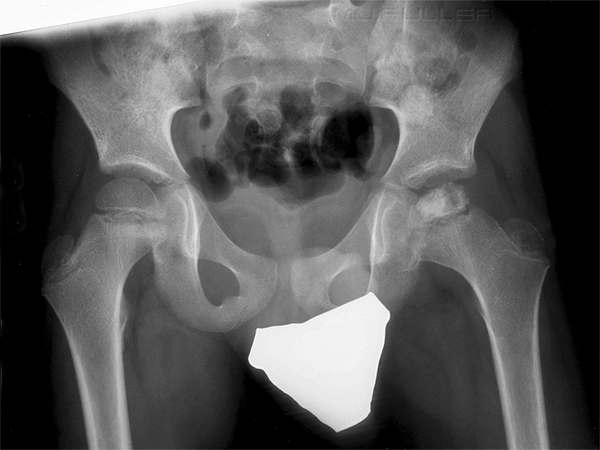
Five radiographic stages can be seen by plain x-ray. In sequence, they are as follows:
- Cessation of growth at the capital femoral epiphysis; smaller femoral head epiphysis and widening of articular space on affected side
- Subchondral fracture; linear radiolucency within the femoral head epiphysis (Crescent, Salter's or Caffey's sign)
- Resorption of bone
- Re-ossification of new bone
- Healed stage (9)
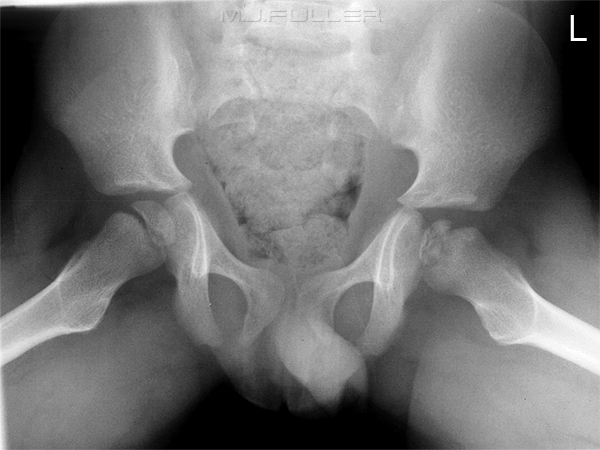
Frogleg lateral
- small left femoral capital epiphysis
- linear radiolucency within the left femoral capital epiphysis
- Wide femoral neck
- widening of the articular space on the left side
Scheuermann's Disease
Wikiradiography Links
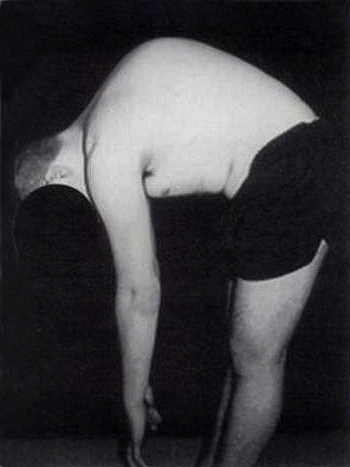
- most common type of kyphotic deformity seen in adolescents
- deformity first described by Scheuermann in 1921
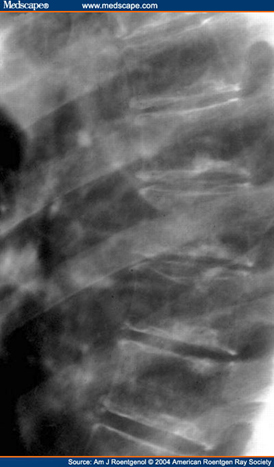
- Characterised by wedged vertebral bodies, irregular vertebral body endplates and increased thoracic kyphosis
- aetiology unclear- mechanical factors (lifting) have been implicated
- herniation of disc into vertebral bodies (Schmorl's nodes)
- narrowing of disc spaces
<a class="external" href="http://www.ajronline.org/cgi/content-nw/full/183/4/949/FIG12" rel="nofollow" target="_blank">http://www.ajronline.org/cgi/content-nw/full/183/4/949/FIG12</a>
Obeneba Boachie-Adjei and Vishal Sarwahi in
Ronald L. Dewald., Spinal Deformities: The Comprehensive Text. Thieme, 2003
References
1. <a class="external" href="http://medical-dictionary.thefreedictionary.com/Osteochondroses" rel="nofollow" target="_blank">http://medical-dictionary.thefreedictionary.com/Osteochondroses</a>
2. S Orava and K Virtanen Osteochondroses in athletes, British Journal of Sports Medicine, Vol 16, Issue 3 161-168
<a class="external" href="http://www.healthofchildren.com/N-O/Osteochondroses.html" rel="nofollow" target="_blank">3. http://www.healthofchildren.com/N-O/Osteochondroses.html</a>
4 <a class="external" href="http://www.latrobe.edu.au/podiatry/Radiology/osteochondrosis.html" rel="nofollow" target="_blank">http://www.latrobe.edu.au/podiatry/Radiology/osteochondrosis.html</a>
5. <a class="external" href="http://www.wheelessonline.com/ortho/osteochondritis_dissecans_of_the_knee" rel="nofollow" target="_blank">http://www.wheelessonline.com/ortho/osteochondritis_dissecans_of_the_knee</a>
Further Reading6. [MASON, MD, MILAN S. MOORE, MD Irregular Ossification of the Tarsal Navicular and Traumatic Midfoot Pain Presenting as Kohler's Disease of the Tarsal Navicular]
<a class="external" href="http://www.wheelessonline.com/ortho/osgood_schlatter_lesion" rel="nofollow" target="_blank">7. Osgood Schlatter Lesion, Wheeless' Textbook of Orthopaedics</a>
8. <a class="external" href="http://www.bgf.asn.au/textbook/diseases/perthes/perthes.html" rel="nofollow" target="_blank">BK Foster, EW Johnstone, Perthes Disease</a>
9. <a class="external" href="http://www.emedicine.com/emerg/topic294.htm" rel="nofollow" target="_blank">Geofrey Nochimson, MD Legg-Calve-Perthes Disease "emedicine"</a>
10. Dr Rajesh Sharma <a class="external" href="http://www.dograrad.com/?p=195" rel="nofollow" target="_blank">http://www.dograrad.com/?p=195</a>
- Waugh, W., The Ossification and Vascularisation of the Tarsal Navicular and Their Relation to Kohler's Disease, J Bone Joint Surg, 1958; 40-B:765-777.
- Williams, G.A. and Cowell, H.R., Köhler's Disease of the Tarsal Navicular, CORR, 1981; 158:53-58.