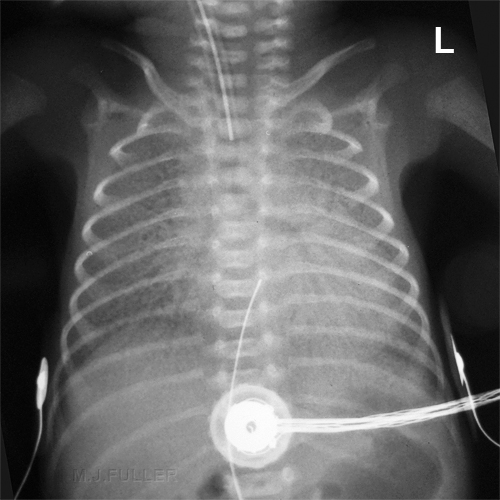
Hyaline Membrane Disease (syn RDS) and BPD
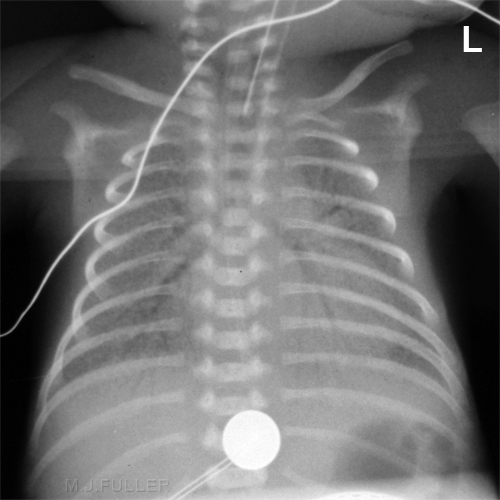
Respiratory Distress Syndrome (RDS) has historically been the chief cause of respiratory failure in premature infants. The same condition is known as Hyaline Membrane Disease (HMD). RDS is due to an inadequate amount of surfactant, a substance produced by the lungs which stabilizes the tiny air sacs in the lungs. In normal lungs at the end of exhalation, a small amount of residual gas remains in the alveoli. Without surfactant, these alveoli fully deflate at the end of each exhalation, and are difficult to reopen in order to fill with air during the next breath. The diminished amount of air-filled alveoli in the lung causes the lung fields to appear dense. However, there may be air in the conducting airways, which are surrounded by the atelectatic alveoli. This relationship between air in the airways surrounded by atelectatic alveoli causes the airways to appear as black branching lines known as "air bronchograms" <a class="external" href="http://www.uen.org/utahlink/tours/tourElement.cgi?element_id=28357&tour_id=15478&category_id=24288" rel="nofollow" target="_blank">Source</a>
X-ray Appearance
- Typically, diffuse “ground-glass” or finely granular appearance
- Bilateral and symmetrical distribution
- Air bronchograms are common
- Especially extending peripherally
- Hypoaeration in non-ventilated lungs
- Hyperinflation excludes HMD
- “Granularity” is the interplay of
- Air-distended bronchioles & ducts
- Background of atelectasis of alveoli
- May change from film-to-film if there is
- Expiration (air disappears)
- Better aeration (small bubble formation)
Respiratory Distress Syndrome (RDS) AKA Hyaline Membrane Disease (HMD)
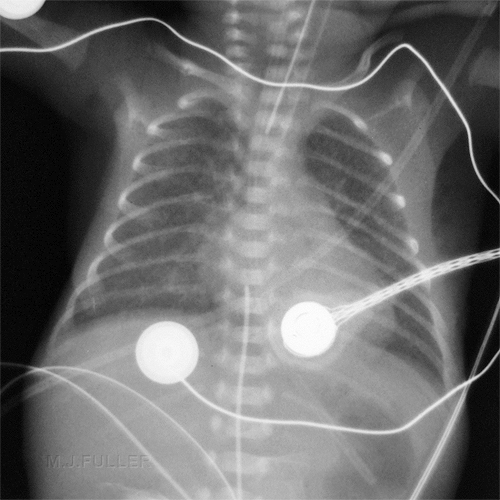
Bronchopulmonary Dysplasia
Same baby as above on day 28
Now showing signs of BPD B
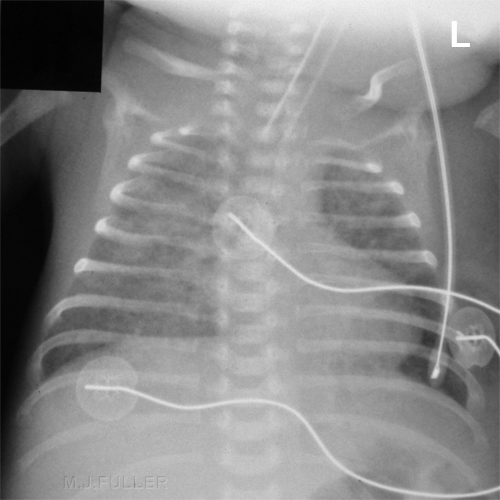
Respiratory Distress Syndrome (RDS syn HMD) and Pulmonary Interstitial Oedema (PIE)
Day 1
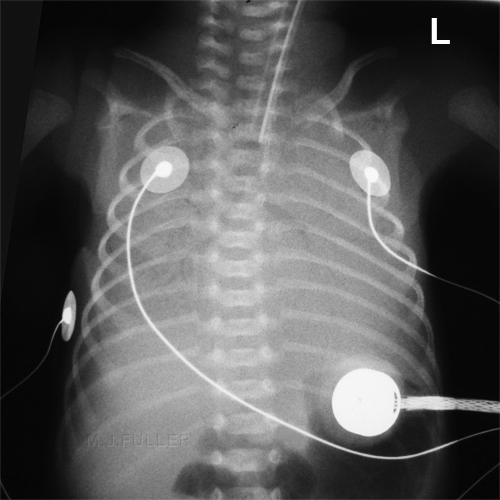
Confluent airspace opacity consistent with hyaline membrane diseaseDay 3
Hyaline membrane disease with focal interstitial emphysema (PIE)